 Our healthcare law firm works with many providers and healthcare practices to assist them in complying with federal, state, and local laws. In particular, our med spa clients often ask whether they can hire medical assistants to perform certain procedures within their med spa. Medical assistants have a defined scope of practice under state law, and having medical assistants perform procedures outside their scope of practice carries legal risk. This blog covers some main points about a medical assistant’s scope of practice, particularly in Georgia. If you are a medical assistant considering to open up a med spa, planning to hire a medical assistant as part of your med spa, or would like to discuss this blog post, you may contact our healthcare law firm at (404) 685-1662 (Atlanta) or (706) 722-7886 (Augusta), or by email, info@littlehealthlaw.com. You may also learn more about our law firm by visiting www.littlehealthlaw.com.
Our healthcare law firm works with many providers and healthcare practices to assist them in complying with federal, state, and local laws. In particular, our med spa clients often ask whether they can hire medical assistants to perform certain procedures within their med spa. Medical assistants have a defined scope of practice under state law, and having medical assistants perform procedures outside their scope of practice carries legal risk. This blog covers some main points about a medical assistant’s scope of practice, particularly in Georgia. If you are a medical assistant considering to open up a med spa, planning to hire a medical assistant as part of your med spa, or would like to discuss this blog post, you may contact our healthcare law firm at (404) 685-1662 (Atlanta) or (706) 722-7886 (Augusta), or by email, info@littlehealthlaw.com. You may also learn more about our law firm by visiting www.littlehealthlaw.com.
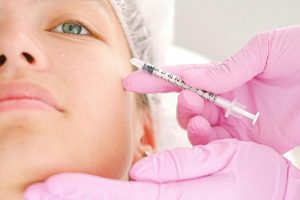
Medical Assistants Are Able to Perform a Very Limited Amount of Medical Tasks Under Georgia Law, and Most Med Spa Services Are Not Within This Limited Amount of Medical Tasks.
The Georgia Medical Board’s regulations outline what medical tasks medical assistants can do. Under the regulations, physicians can delegate the following tasks to medical assistants: Continue reading ›